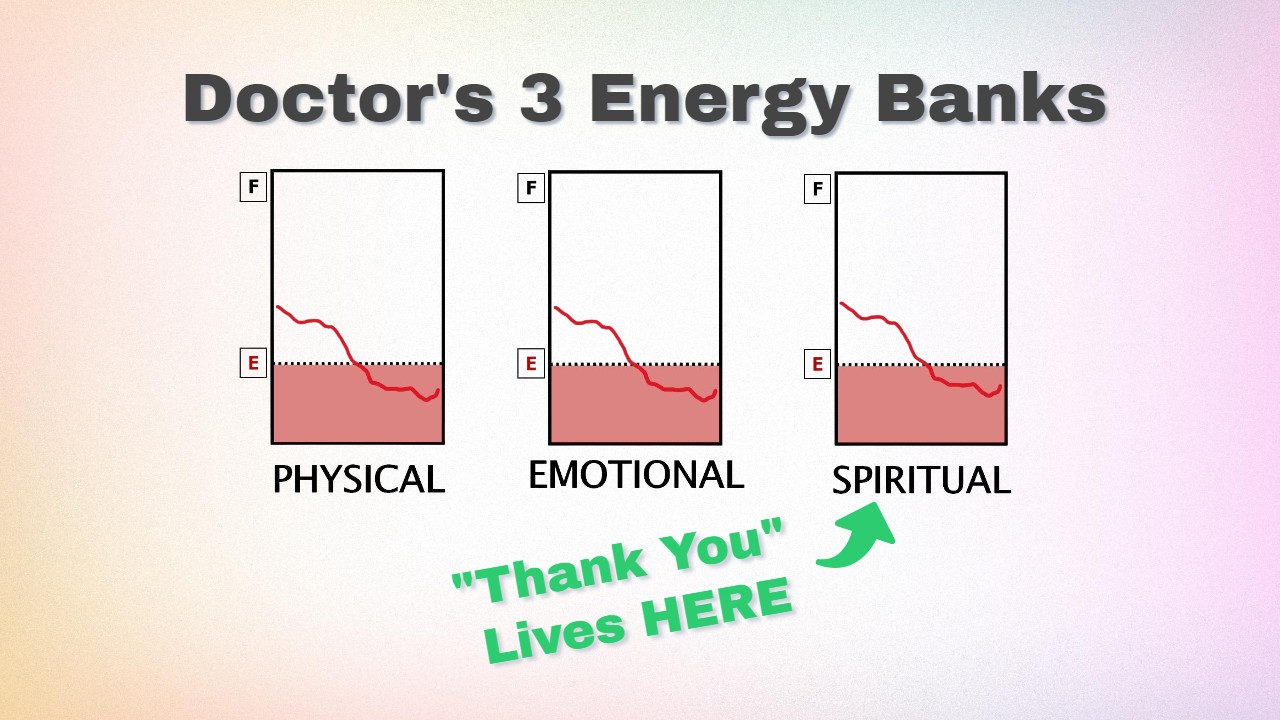
To prevent physician burnout, you must manage your three internal Energy Banks
A Thank You from a patient or family member can top up all three accounts, but ONLY if you know what to do and say in that moment.
"Thank You" is like rocket fuel because it provides an instant infusion of Spiritual Energy, reconnecting you with the purpose in your practice.
Unfortunately, most doctors deflect thank yous and miss this golden opportunity to prevent burnout.
This is another lesson we never received in Med School, Residency or Fellowship - How to RECIEVE a Thank You with Elegance and Grace.
NOTE:
This is Part 3 of 3 in our Series on Physician Energy Management. Here are the first two:
Part 1 - Physician energy has nothing to do with batteries being run down
Part 2 - Physician's 3 Energy Banks
Physician's Top 3 Work-Life Balance Shortcuts
FREE Online Video Training >> Lessons from our 40,000 doctor experience
5 CME Credits - Short Online Video Lessons
Tools for Daily, Weekly and Monthly Balance
The Thank You Connection to Spirit
Spirit in your practice is your connection to PURPOSE. You must have reminders you are making a difference and serving a purpose regularly or your Spiritual Energy Bank becomes drained. At that point, the little voice in your head might start whispering, "What's the use."
That little voice phrase, "What's the use. I'm really not making a difference or serving a purpose here," is actually the third symptom of burnout.
Here's how I discovered the Thank You connection to Spirit.
It was by accident, early in my physician coaching practice. I was looking for a way to help doctors remember what they enjoy about seeing patients
I asked hundreds of my physician clients:
"Tell me about your last Ideal Patient Visit"
You know the one...
That special interaction, during an otherwise busy day, that lights you up. Where, at the end of the day, you said to yourself,
"oh yeah, that's why I became a doctor in the first place," with a little fist pump.
Or when you get home, you say, "Honey, sit down, I have to tell you what happened at work today."
About ten doctors into this inquiry, a pattern began to emerge that has held true to this day - across hundreds of doctors.
97% of the time that feeling of satisfaction and accomplishment comes from two words the patient, or a family member, said to you.