 Physician Burnout – British NHS Announces World’s First Government "Burnout Service"
Physician Burnout – British NHS Announces World’s First Government "Burnout Service"
The British National Health Service (NHS) has been having a very rough time lately. Despite always being mentioned as one of the top healthcare systems for cost effectiveness, they are fighting a running battle with rampant physician burnout and a near mutiny by providers. Here are just a few of the low points.
- Burnout rates are sky high
- The providers will strike the government every month for the rest of this year over an attempt to force a standard 7-day work week
- There is even an effort to get doctors to turn in their colleagues for burnout
Now the government is attempting a turnaround
Last week the NHS announced that beginning in 2017 it will spend £19.5 million ($24M USD) in 2017 to treat burnout in General Practitioners (GP’s) nationwide.
The NHS announcement said:
“The service is the world’s first nationally-funded health service of its kind for general practice, a clear signal of NHS England’s commitment to help retain a healthy and resilient workforce and in supporting GPs and GP trainees who wish to remain in or return to clinical practice after a period of ill health.”
The service is described as follows:
“Under the service, GPs will be able to access face-to-face support across 13 regions in England for general psychiatric assessment and treatment, addiction related health problems and one-to-one and group psychotherapy sessions.”
============
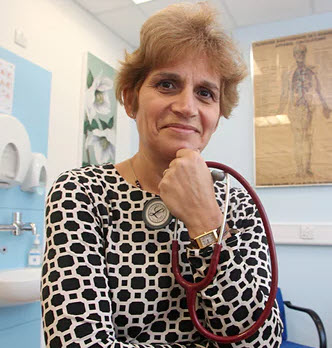 Dr. Clare Garada (otherwise known as Lady Wessely) is the current head of the NHS Practitioner Health Programme (PHP). She is a London-based general practitioner and former Chair of the Council of the Royal College of General Practitioners. She went on to say:
Dr. Clare Garada (otherwise known as Lady Wessely) is the current head of the NHS Practitioner Health Programme (PHP). She is a London-based general practitioner and former Chair of the Council of the Royal College of General Practitioners. She went on to say:
"This really is good news, it’s the first time - I think anywhere in the world - that public money has been put toward supporting a profession in this way.
And we’re going to try and develop, right from prevention to treatment, a whole range of services right across the country."
============
We agree -- this is a great first step -- and it is NOT a prevention program for Physician Burnout by any means
This program is structured to diagnose and treat psychiatric complications of burnout.
They specifically describe psychiatric assessment and psychotherapy. Burnout is not a psychiatric illness. Depression, alcohol and drug abuse and disability are complications of physician burnout. Let me be clear here ...
Physician Burnout is a NORMAL RESPONSE to overwhelming stress in the workplace
YES, you definitely need a crisis intervention program like this.
It is a crisis management and suicide prevention maneuver - something that is very important in the toxic environment of the NHS. Doctors must have a physician specific hotline and a way to ask for help when they are over the edge.
But PLEASE DO NOT STOP THERE.
On the physician side, they need resilience support:
- What about completing the doctor’s medical education about stress, stress management and burnout?
- What about teaching them the four causes of physician burnout?
- What about teaching the truth that physician burnout is not a problem – and why it is so important to stop looking for a solution?
- What about giving them the 117 ways to prevent physician burnout so they can build their personal prevention strategy.
Let’s go right at physician burnout with a prevention campaign rather than focus only on those physicians whose burnout has driven them to depression, alcohol, drugs and thoughts of suicide.
Without a parallel prevention program and – most of all – a concerted effort to detoxify the healthcare workplace in Britain, this new crisis management program could go on forever and not make a dent in the annual number of physicians who will utilize their services.
 Remember, physicians are the canary in the coal mine of medicine
Remember, physicians are the canary in the coal mine of medicine
This program is rescuing the canary after it has fallen limp and unconscious to the floor of the cage, nursing it back to consciousness and then stuffing it right back into the same toxic mine. Yikes!
An effective burnout prevention program would do two things:
1) Build a Stronger Canary – provide prevention and resilience training as outlined above -- filling the holes in the doctor's medical education around stress, stress management and burnout.
2) Detox the Mine – systematically redesign the workplace to lower the stress on the workers.
Unfortunately, this program – even with its £19M pound price tag does neither.
You Can Help Us Help the NHS
We have the tools to show the NHS how to build a true system-wide, proactive physician burnout prevention program.
Full Disclosure:
I spent my high school years in the Midlands of England -- learned to play rugby and drink warm beer there. I even have 8 "O Levels" and friends back in "the old country".
I have been itching to do a pilot project with the NHS for years. It has been like watching a fatal car crash in super slow motion knowing the end result -- and I would love to show them what we have proven to work on this side of the pond.
If you know anyone inside the leadership of the NHS and could provide an introduction, we would really appreciate it. Hit this link and contact me immediately please.
The NHS must be shown effective prevention tools so they don’t think treating the walking wounded is the only way to cope.
============
PLEASE LEAVE A COMMENT:
What do you think about this program, its focus and its chances to have a significant impact on physician burnout in the NHS?

